I have been reading research papers and news articles since the beginning of the pandemic. I have isolated from my spouse twice when I thought I might have it. Based on that, here is my advice on what to do if you get COVID-19, what research says are good ideas, and how to prepare for being sick.
(Note that this advice assumes that you have a mild case (i.e. are recovering at home). If you do get hospitalized, then doctors will pay attention to you.)
- Stay away from your loved ones until you test negative. This doesn’t help you recover faster, but it would suck for you to need to take care of your loved ones while you are still recovering. Be quiet if you have to be around them.
- Stay entertained.
- See if you qualify for Paxlovid. Note that the research says that you have to take Paxlovid as soon as possible, you can’t “wait and see”.
- Most people report that Paxlovid leaves a bad taste in the mouth.
- This article (2025-04-30) says that having any food in your mouth blunts the bad taste.
- This Mastodon posting (2025-07-16) says that chocolate in particular blunts the taste (and implies that you don’t have to eat it continuously).
- This first-person account (2022-06-24) says that cinnamon candy is the thing to get.
- Most people report that Paxlovid leaves a bad taste in the mouth.
- Other meds/supplements you could try (see my Treatments page for references):
- There’s quite a lot of research that says that antihistamines (especially H1 antagonists) work well as COVID-19 treatments and preventatives.
- I have not found an over-the-counter nasal chlorpheniramine in Canada or the USA, but there *are* some other H1 antagonist antihistamine nasal sprays which are available over-the-counter in the USA.
- Astepro nasal spray, active ingredient azelastine (first generation H1, i.e. crosses the blood-brain barrier)
- Livostin Nasal Spray, active ingredient levocabastine (second generation H1, i.e. does not cross the blood-brain barrier)
- I have not found an over-the-counter nasal chlorpheniramine in Canada or the USA, but there *are* some other H1 antagonist antihistamine nasal sprays which are available over-the-counter in the USA.
- If you can get a doctor’s attention and convince them, multiple research papsers say that metformin cuts the risk of Long COVID by about half, and reduces the risk of a severe infection by ~16%.
- This paper from Germany (2025-05-12) reports that 4 weeks of 1000 mg/day of Vitamin B3 helps both the acute phase and prevents Long COVID. People on B3 were 35% more likely to have their symptoms fully resolved at the end of two weeks.
- There is some research that licorice root extract is useful against COVID-19.
- This page from RTHM.com has suggestions for meds and supplements to take.
- There’s quite a lot of research that says that antihistamines (especially H1 antagonists) work well as COVID-19 treatments and preventatives.
- There’s really good research that says that irrigating your sinuses (at least) twice per day with saline solution works exceptionally well.
- Make sure you have good air: clean, warm, and between 40 and 60 percent relative humidity.
- Take probiotics.
- There’s one paper which says that taking the probiotic Lactococcus lactis drops the risk of losing smell/taste by 78%. (This probiotic is common. Costco’s probiotic capsule has it.)
- Don’t try to do too much when you spring yourself.
Tell People
Tell all the people you were in contact with for the previous week, so that they can measures they think are appropriate.
Isolate until you test negative (then mask!)
The US CDC says to isolate until five days after your first symptoms. The BC CDC says that if you are fully vaccinated, you can stop isolating after five days if your symptoms improve and you don’t have a fever. This is utter bullshit. There are lots of studies which say that most people are still infectious until 7-10 days after symptom onset:
- This preprint from the USA (with samples taken during the early Alpha period) (2022-09-27) found they could grow viral culture from participants for a mean of 11 days;
- This paper from USA (2023-02-08) found that 17% of participants had culturable virus after 5 days; the longest someone was culturable was 12 days.
- This preprint from the UK (with samples taken during the Delta/B.1/B.2 period) (2023-03-09) found that people had high enough viral load to be infectious for 7-10 days. They found no correlation of symptom severity with viral load.
- This preprint from the USA (with samples taken from July 2021 to January 2022) (2022-03-02) found a median of 6 days from positive test or start of symptoms to no longer cultureable, although 15% of participants’ swabs could culture virus for more than 10 days.

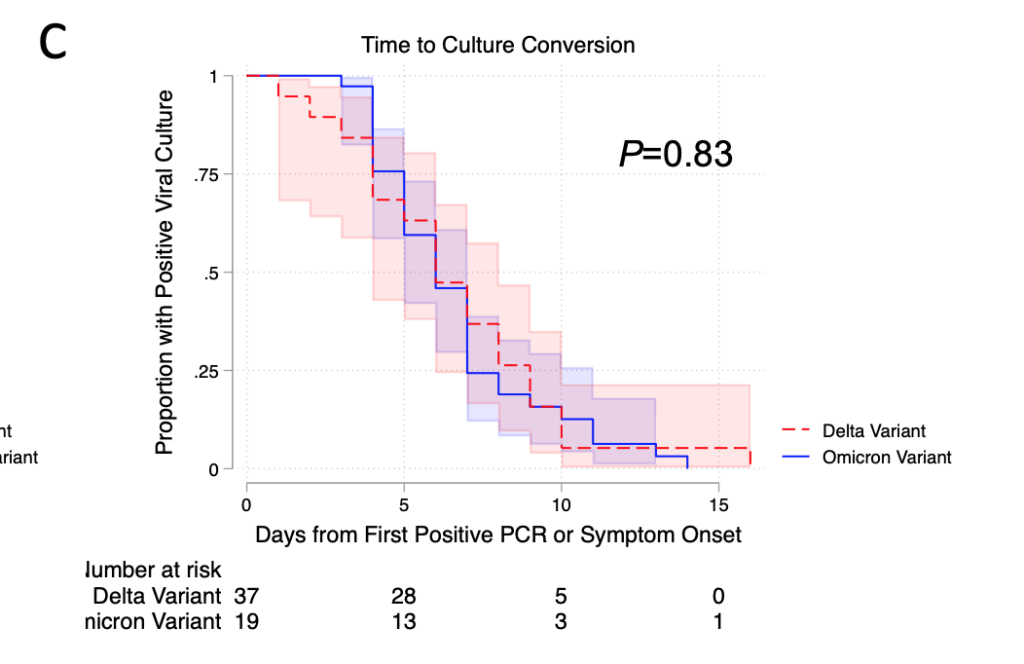
I believe that I have seen more papers than the three mentioned, but they are a little hard to search for.
Now, rapid tests are notoriously unreliable, especially when the viral load is low. This is why you should mask for a while after you test negative. Even if the rapid test says you are good, you will probably be less contagious, and with a good mask (use an N95-class!), you should be good.
Isolate from your Pets
Note that you should isolate from your pets as well (sorry!). Dogs and cats can catch COVID-19! Cats are especially susceptible (see also this and this and this); it can be fatal. Dogs have been shown to get cognitive damage, just like humans.
There have been documented cases of cats transmitting COVID-19 to humans. I don’t know of documented cases of dog-to-human transmission, but that doesn’t mean it doesn’t happen.
When Can I Leave?
Given that Rapid Antigen Tests are so flakey at low virus levels, how do you know when you test negative? Do you need a PCR test before you can go out? Well, that’s not practical, since almost nobody in Canada can do PCR-quality tests without going out. (Though note! Metrix claims that approval for their NAATs in Canada is coming soon. Email them at sales@aptitudemedical.com to get on their waiting list.)
If you get a positive RAT, you still need to isolate. Period. Your levels are high, and you are a danger to other people.
On the other hand, while a negative RAT test does not mean you are shedding zero, it does mean your levels are low. You are less likely to infect other people. If you do go out right after a RAT, please please please wear a mask to protect other people. (And don’t go see anybody vulnerable.) It’s probably best to wear a mask for five days after your last positive test.
Furthermore, a negative RAT after a known infection is better news than a negative RAT when you think you are healthy. At the beginning, your infectiousness is increasing and after an infection, it is decreasing. If you think you might be coming down with COVID-19, take a RAT at 9AM, and it’s negative, it might be that you are infected, and at 1PM, your loads might have gone up enough to get someone sick. If you’ve been sick, you take a RAT at 9 AM, and it’s negative, then you will be less infectious at 1PM. Unless you have a rebound.
While there is conflicting research on whether Paxlovid makes you more likely to have a rebound, you can have a COVID-19 rebound even if you are not on Paxlovid. Be aware, and keep testing for a few days after you think you are done.
Be quiet
There was one paper (note: just one) which said that they couldn’t find any culturable virus from the breath of people who were “tidal breathing”, i.e. just sitting there, not exercising, not talking / singing / yelling / coughing / sneezing.
There are other papers which found SARS-CoV-2 RNA in exhaled air, like this one. It seems unlikely that 100% of the exhaled RNA would be dead virus, but the alternative is that the paper above it is just wrong. 🤷♀️
This older Letter to the Editor (note: which means it is not peer-reviewed) (2025-07-15) hypothesizes that people get infected in the nose and then later speak, generate aerosols, and breathe their own aerosols into their lungs, making their disease worse. They interviewed Deaf people about how much they wore masks, how much they vocalized, and how severe their COVID-19 infections were. They found that the more the deaf patients wore masks, the milder their symptoms; the less they vocalized, the milder their symptoms!
Stay entertained
Early in the pandemic, I used to say, “It turns out that love is stronger than fear” as people broke quarantine rules around the world to spend time with loved ones. Now, I say, “Boredom is stronger than fear” as I have seen responsible, caring, intelligent people I know go places after five days, even knowing that they were probably still infectious after five days. (They knew because I told them and gave them references.)
I also have isolated twice, once early on when I had COVID-like symptoms and once recently when I was exposed. It’s hard!
The most important things you can do to keep from infecting your loved ones is to stay isolated, but you aren’t going to be able to do that if you are bored out of your skull and/or frantic for physical exercise. If you have someone to help take care of you, have them bring you entertaining stuff. Better yet, arrange this ahead of time. (See later on for my ‘how to prepare’ list.)
Walking around outside, especially if you have a mask on, is pretty low risk for other people. Do wear a mask when going from your room to the door, and preferably have your roommates be far away. (I can’t go outside when isolating because I live in an apartment building where I can’t get up to my floor without getting into a small poorly ventilated room an elevator.)
Don’t go out if you are sneezing or coughing, please. It is really really difficult to restrain yourself from lifting your mask to cough/sneeze (because yeah, that’s gross), but that’s exactly the time when the mask is needed. Pro tip: if you feel a sneeze coming on, tickle the roof of your mouth with your tongue and that will inhibit the sneeze. You’re welcome.
Paxlovid
If you are eligible for Paxlovid (BC rules, USA rules), and don’t have drug interactions which would conflict, get on the phone immediately to your doctor to talk about Paxlovid. Paxlovid works really really well, but you have to start within five days of getting symptoms.
Rinse your sinuses
There’s research that says that irrigating your sinuses (with something like this) works even better than Paxlovid. No lie. (I’m not suggesting you irrigate instead of Paxlovid, you can do both.) (Note: put baking soda in as well as salt, it will feel much nicer. I use a .25 tsp to .25 tsp to 500 mL water salt:baking soda:water mix.)
Here’s the evidence:
- This paper (2022-08-25) found that irrigating sinuses with saline or povidone-iodine after getting infected cut the hospitalization rate in people over 55 by 8.57 TIMES. Not 8.6%, 8570% percent. (They saw no difference between saline and povidone-iodine, so use salt, it’s easier.)
- 2023-11-08 This paper from USA says that people who gargled and irrigated their nose with saline had ~1/3 the hospitalization rate of controls.
- This paper from USA (2023-11-08) found that people who gargled and irrigated their noses with saline had a hospitalization rate of about one third that of controls.
- This paper (2021-12-15) on a study of hospital workers in Mexico found that 1.2% of workers who did nasal rinses with neutral electrolyzed water got COVID-19, compared to 12.7% in the control group who did. That’s a 10x difference.
- This paper (2020-09-11) found that people who irrigated with saline got over COVID-19 symptoms in about 10 days vs. 14 days for people who didn’t.
- This small study (2021-02-04) from France early in the pandemic found that after sinus rinse with povidone iodine (not saline!) all the COVID-19 patients in the study but one tested negative after three days.
- This paper (2021-03-27) doesn’t give results, it just tries to explain what the helpful actions of nasal irrigation are (at a cellular level).
- This small study (2019-01-31) pre-pandemic of people with “common colds” found that people who did nasal irrigation and gargled resolved symptoms 1.9 days before those who did not and reduced household transmission by 35%. (Note that many “common colds” are coronaviruses!)
I have had a number of people express extreme hesitancy about sinus irrigation. “I remember getting salt water / pool water up my nose, and it was horrible!” Yes! Getting salt water / pool water / tap water up your nose is absolutely horrible: 0/10, would not do again. However, the salt + baking soda that you put in your irrigation water means that it doesn’t hurt at all. It’s a little weird, but it does not hurt. (You do want to use distilled water or boiled water for safety reasons.)
Nasal Sprays
Nasal sprays are like irrigation-lite.
- This paper from UK (2025-10-09) reports that people who had a history of co-morbidities or a history of lots of respiratory illnesses who used either Vick’s First Defence or isotonic saline nasal sprays six times per day for twelve months had 18% fewer sick days than those who did not use nasal sprays.
- This paper from UK (2024-07-11) reports that people with COVID-19 infections got better about 1.7 days faster if they sprayed twice per day with either a gel-based spray or a saline spray. (Note: this was not a full irrigation!)
Rinse your throat
This paper gives a theoretical argument for rinsing your mouth reducing how severe your illness is. The basic idea is that if you’re sick, you’ve got a bunch of germs in your mouth; you might as well kill them off. I haven’t seen any controlled trials which look at mouth rinsing by itself, but some of the nasal rinse trials included gargling or oral rinses. Most importantly, oral rinsing is a very low-risk activity.
If you want to swish and spit, the paper says to do it for 60 seconds. A dilute hydrogen peroxide solution (1-3%) looks like it’s best. Colgate Peroxyl is a commercial brand of H2O2 if you don’t want to mix your own.
I haven’t seen any papers which rank salt solutions, but I wouldn’t be surprised if saline is reasonably good, based only on what I’ve seen in the nasal rinse literature.
If you want to read up on the studies, go see my Treatments page and search for “mouthwash”.
Help your cilia / Good Air
I am not a doctor, but the picture I have put together in my head is that the cilia in the respiratory tract are like little conveyor belts which take bacteria and viruses out. If your cilia get gunked up with crud, or get damaged, then they can’t take out the COVID-19 viruses as well. (Similarly, if they are full of COVID-19, when you do a nasal rinse, you take out a bunch of the garbage for them, and make it easier for them to take the rest of the garbage out.) Help your cilia! Reduce the amount of gunk you breathe in and keep them happy!
Low particles
There have been lots of studies which have shown that air pollution (like, oh, say, smoke from wildfires) is really bad for COVID-19, and the effects are not small. When air quality in an area is poor, more people catch COVID-19 and they have more severe cases. The studies disagree on which aspect of the air pollution is most responsible, but they all say air pollution IS BAAAAAD:
- This paper from China (2020-06-08) says air pollution is bad, humidity is good.
- This paper (2021-05-22) says that air pollution is bad for COVID-19, with different correlations at different times.
- This paper from the USA (2020-10-15) says that each 4.6ppb increase in NO2 made the COVID-19 case-fatality rate and mortality rate go up by 11.3%; a 2.6 μg/m increase in PM2.5 made the mortality rate go up by 14.9%.
- This paper from Sweden (2023-03-07) says that the higher the PM2.5, the higher the risk of Long COVID is.
- This paper from the USA (2020-09-11) says that “an increase in the respiratory hazard index is associated with a 9% increase in COVID-19 mortality”.
- This paper from China (2020-04-18) found that a 10-μg/m3 increase in PM2.5, PM10, NO2, and O3 was associated with a 2.24%, 1.76%, 6.94%, and 4.76% increase in the daily counts of confirmed cases.
- This paper using data from China, Italy, and the USA (2020-04-16) found that NO2 correlated with per capita cases (tau .12-.52, depending on the country). PM2.5 had a weaker correlation (tau .08-.31). PM2.5 correlated to mortality (tau .14-.19)
- This paper from Italy (2020-05-05) says that “long-term air-quality data significantly correlated with cases of Covid-19 in up to 71 Italian provinces”.
- This paper from the USA (2020-04-27) says that “an increase of only 1 μg/m3 in PM2.5 is associated with an 8% increase in the COVID-19 death rate”
- This paper from Spain (2023-04-05) says that people who have long-term exposure to polluted air have lower antibody responses to vaccination.
I bumped into this paper from the USA which talked about how nasty the air is in open-kitchen restaurants. Apparently, grilling and frying meat gives off a ton of particles. (This makes sense; it sometimes gets smoky in the kitchen when you are cooking. Those are particles!) This explained something which I had heard but didn’t understand: line cooks have the highest mortality of all the occupations. You’d think it would be meatpackers or health care workers, but no. Cooking makes particles, and PARTICLES ARE BAD FOR COVID-19!
If you need more proof that air quality is important, check out this tweet: air pollution is the fourth-leading risk factor for death in general:

Humidity
There have been a number of studies (like this one) which found that COVID-19 likes really dry air or really wet air. Keep your relative humidity between 40 and 60 percent.
- This page gives arguments for humidity of 40 to 60 percent in infographic style.
- This paper says that cilia took 63% longer to transport gunk out in dry air.
- This article says that 40 to 60% relative humidity is the sweet spot.
- This article talks about a study where one nursing home kept the relative humidity between 40 and 60 percent and lost zero patients; a home two miles away which did not regulate humidity lost a 10% of their residents.
- This paper found that low humidity led to higher COVID-19 rates.
Warmth
This article, reporting on this paper, says that cold ambiant air temperatures — even a drop of five degrees C — decreases your nasal immunity significantly. So keep your air warm! (Note that wearing a mask will warm your air.)
Probiotics
There are now a number of papers which say that the gut biome gets messed up by COVID-19. Several explicitly say that taking probiotics is useful. See this Twitter thread for a summary of papers.
Take aspirin, maybe?
This paper looked at patients who had been on anticoagulants (like aspirin) (presumably for cardiovascular issues) before going into the hospital with COVID-19 versus controls. (However, see below.) They used matched controls, but even so, the anticoagulant cohort was sicker — but did better! And the subgroup who had their anti-coagulants stopped when they went into hospital did much worse than the group that kept taking them.
Now, not only am I not a doctor, and this study was not designed to look at generally healthy people who caught COVID-19, but it does make me wonder if aspirin’s anti-inflammatory properties are a good thing. On the other hand, maybe they are only a good thing once you get in really bad shape (and anti-inflammatories do give a higher risk of bleeding out if you get cut).
However, this paper from Peru (2025-07-11) found tha self-medicating with aspirin increased the risk of COVID-19 infection by 134%.
Fever Reducers
This Comment (<- not peer reviewed!) says that taking non-steroidal anti-inflammatories doesn’t seem to have an effect on COVID recovery. The Mayo Clinic says that adults don’t need to take fever reducers until they’ve got a fever of 102. Understand that fevers are in some ways, a good thing: your body can generally tolerate higher heat than viruses and bacteria can, and the immune system actually functions better at higher heat.
Also: Acetaminophn/Tylenol is dangerous.
NB: Yes, aspirin is also a fever reducer, in addition to being a mild blood thinner. The section above which says that taking aspirin might be good was talking about its anti-coagulant role.
Take it easy!
There was one kind of throw-away sentence in an abstract of a study on Long COVID which said that not taking it easy after recovering from COVID-19 correlated with getting Long COVID. I remember that, but I’m sorry to say that I can’t find the paper.
It was only one paper, and I don’t know how they justify the claim. However, it makes sense to me, is relatively cheap and easy to do (compared to like, spending a week in a hyperbaric pressure chamber or something like that), has very few side effects, and I have seen anecdata about taking it easy being good on Teh Socials.
Preparing ahead of time
Once you are sick, there are things I mention above which you will not be able to do for yourself. If you have family or friends who will take care of you, you can offload some stuff to them. Or you could use DoorDash or something like that — but it’ll be easier if you prepare ahead of time. If you can, I would make sure you have these on hand:
- High-quality N95-class masks. These will help keep your household members safe if you have to make brief dashes into common areas. They will also help you if the air quality sucks and you don’t have an air filtration device.
- Sinus irrigation kit and 4 litres of distilled water. The NeilMed kits are about CAD$20 at just about any pharmacy. Yes, they are a total rip-off — twenty bucks for a plastic bottle and some salt and baking soda?!?!? However, their value is much higher than their price.
- If you can find another bottle that will work, good for you, use that. Put equal parts baking soda and salt into a bottle, shake really really well, put 1/4 teaspoon into 250 ml of water, and irrigate away.
- Particle detector and air filtration device.
- This is the particle detector I got, though I got it from the US.
- Spouse and I built a Corsi-Rosenthal box (cost ~CAD$200) which works really well. During the recent wildfire smoke, it took the PM2.5 count in our living room from 47 µg/m^3 to 12 µg/m^3 in 17 minutes. (NB: I had a hard time finding a 20″ box fan on short notice when we were making ours.)
- Here’s a mini Corsi-Rosenthal box.
- Here’s a tweet thread talking about making a thinner box with computer fans.
- Entertainment. Netflix? Books? Art supplies? Videogames? This is going to be highly individual.
- Possible medications:
- All your normal medications.
- Paxlovid, if your doctor so advises.
- Metformin, if your doctor so advises.
- Antihistamines, especially H1 antagonists like Claratin.
- Regarding fever reducers, don’t just take them willy-nilly: fevers are your friend! Fevers make it harder for viruses to operate and make your immune system work better. However, if your fever is too high, then you can have really serious problems. So have some on hand, but don’t take them too soon!
- Licorice root extract, perhaps. (See my Treatments page.)
- Vitamin C, perhaps. (See my Treatments page.)
- Physical activity equipment. This might be weights, a jump rope, a hula-hoop, a stepstool, dancercize videos, Wii, whatever. Just something that will help you move your muscles a little.
- Probiotics.
- A humidifier.
Prevention
What can you do to keep from getting sick? Stay up-to-date on boosters (get one every four months if you can) (and get your shot in the evening and in the same arm each time), avoid crowds, wear masks indoors, all the stuff which public health used to tell you to do. (Exception: I have seen nothing to convince me that washing your hands a lot reduces your risk of COVID-19. Washing your hands is a good idea in general: it lowers your risk of other nasties.)
One thing that public health has not mentioned is to get exercise (before you get sick). This paper and this paper, both from the USA, say that the more physical exercise someone gets (up to 150 minutes per week), the milder their COVID-19 infections will be.
Furthermore, there seems to be good evidence for nasal irrigation and some evidence for oral rinses as preventatives.
Afterwards: Long COVID
If you don’t get better (or you get better and then get worse again!), see this excellent Long COVID resource guide. It’s slightly US-centric, but most of the info will be good for you.
This booklet put out by the World Health Organization gives tips for recovering and/or coping with symptoms after the acute phase.
This paper from Greece (2025-04-24) reports that 0% of patients who took a dietary supplement containing glucosamine sulfate and fucoidan for four months, starting two weeks after a COVID-19 infection, got Long COVID, compared to 21.4% of the patients who got a placebo.
This paper with data from Honduras (2024-11-26) reports that people who are people who took intranasal chlorpheniramine — a first-generation H1 antagonist antihistamine — right away after they tested positive for COVID-19 had many many fewer Long COVID symptoms, as seen in the chart below.
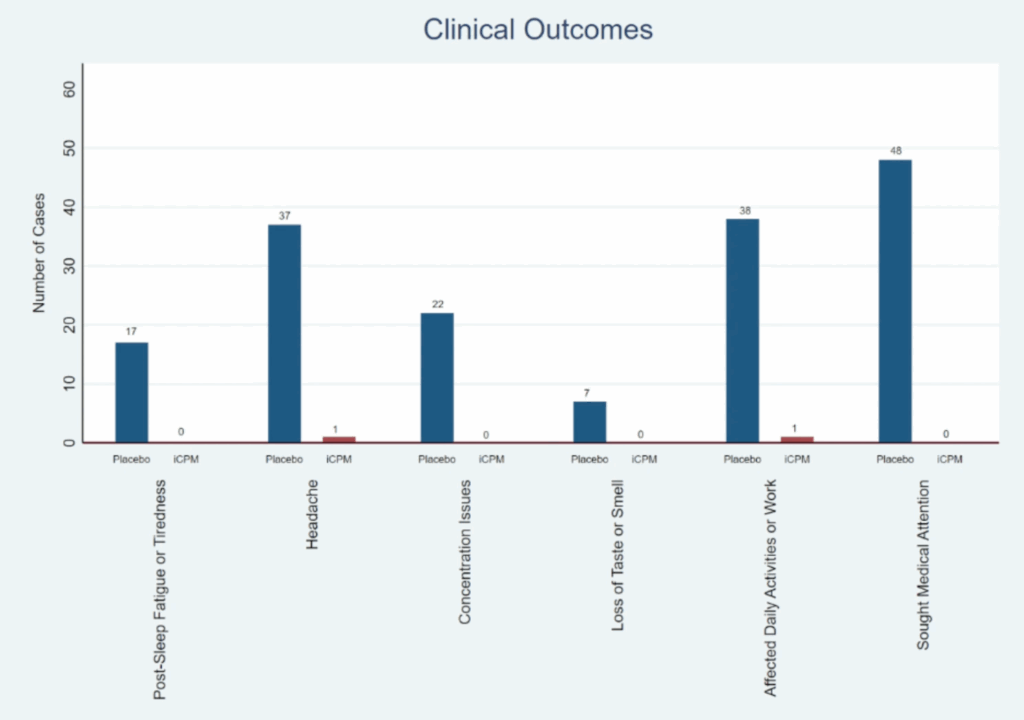
The red bars that you can’t hardly see are the people who got the nasal spray.
Patients got 100 µL of the solution per nostril three times a day using a 1.0% chlorpheniramine solution.
Further Advice
- Other treatment advice:
- This article by a pharmacist, describing what she thinks of various drugs for COVID-19 in great detail. (Interestingly, she also recommends saline nasal rinses, although she doesn’t explain why.)
- I also collect information on treatments. It’s not a very well laid-out or maintained page (yet), but I’m working on it.
- Other people’s acute care advice:
- This Violet Blue page has a section on what to do if you catch COVID.
- What to do when I have COVID (unknown author).
- What to do when you get COVID by Monkeys on Typewriters.
- What To Do If You Catch COVID (video, pretty generic) by Roots.
- Basic Acute COVID Care 101 by plague prose.
