Multiple Pathogens
Vaccines
🎉🎉🎉👃🐁 You might have read articles like this one (2026-02-19) about this paper (2026-02-19) reporting the development of a nasal spray that protected mice for at least three months from a lot of different respiratory diseases, including SARS1, COVID-19, a bat coronavirus, and at least two bacteria. It even quieted reactions to dust mite allergen.
This treatment is similar to this paper (2025-08-13) which I wrote about in my 2025-10-06 blog post. That paper, from a different lab, has a slightly different approach, but both work — as near as I can tell — by increasing the activity of the innate immune system.
The bad news is that, if I understand correctly, both of these treatments will increase inflammation, and long-term inflammation is generally bad for you as this article (2024-01-03) describes. In addition to some shorter-term effects, chronic inflammation increases your risk of heart disease, diabetes, and cancer.
Still, there are some situations where a universal vaccine would absolutely be awesome. For example, if everybody in Wuhan had taken a universal vaccine at the start of the COVID-19 pandemic, we would be in a lot better shape today. Doctors going off to treat Marburg or other nasty hemorrhagic fevers sure would like that kind of protection.
Just don’t think you’re going to take a 3-month universal vaccine every three months.
Pathogen-Related Excess Sickness and Death
This paper from Denmark (2026-01-23) reports that if a mother gets an infection while pregnant, that baby has a 46% higher risk of a suicide attempt when it gets older. (It’s almost like pathogens are bad for you!) The father getting an infection didn’t affect his child’s suicide risk. (The paper is paywalled, so I couldn’t see what kinds of infections, but I suspect that it’s usually respiratory infections just because those are the most common kind of infection.)
Recommended Reading
💉 This post (2026-01-07) is a long, but very nice article on the history of vaccine development.
COVID-19
COVID-Related Excess Sickness and Death
🛌 This preprint from USA (2026-02-15) reports that COVID-19 infections increase the risk of new-onset obstructive sleep apnea (OSA) diagnoses. Compared to COVID-negative controls, hospitalized COVID-19 patients had a 41% higher risk of OSA and non-hospitalized patients had a 33% higher risk.
This paper from USA (2026-02-24) reports that COVID-19 infections increased the risk of kidney issues, while influenza did not. Compared to people who didn’t have either COVID-19 or influenza infections, people who got COVID-19 infections had:
- +174% higher risk of acute kidney injury (AKI);
- +39% higher risk of chronic kidney disease (CKD);
- +222% higher risk of end-stage renal disease (ESRD);
- +28% higher risk of glomerular diseases.
Influenza had no impact on CKD, ESRD, and glomerular diseases. (That implies that influenza did have an impact on AKI, but the paper was paywalled hard enough that I couldn’t see what the impact actually was.)
You might have recently seen an article (like this one (2026-02-26)) saying that young people in the US are having more heart attacks and said to yourself (because you read this blog), “AHA! I bet that’s COVID!” No, actually, this time it is not COVID-19. It’s been a trend since well before the pandemic, and there wasn’t a jump when the pandemic started.
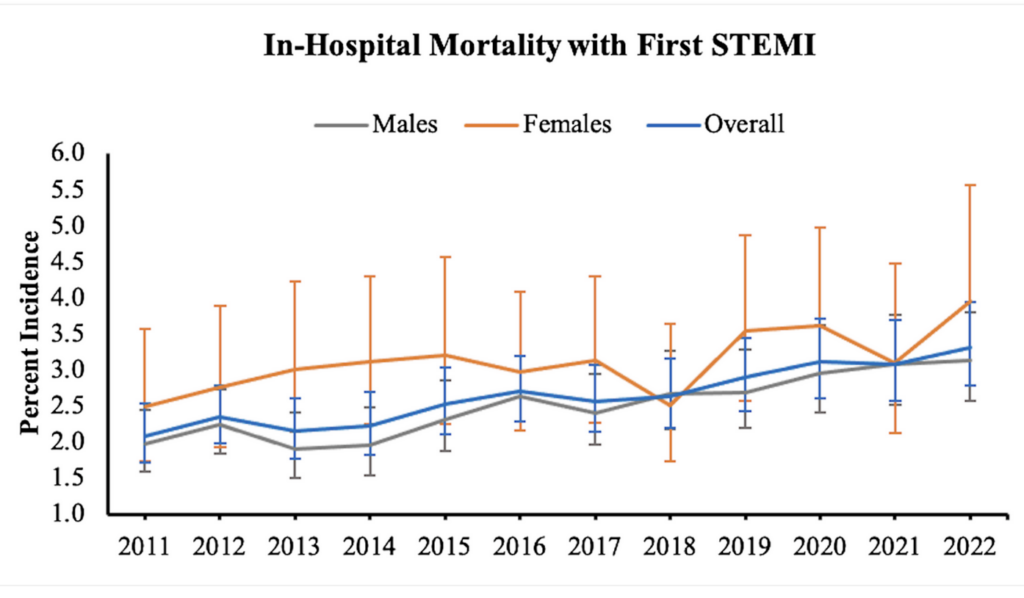
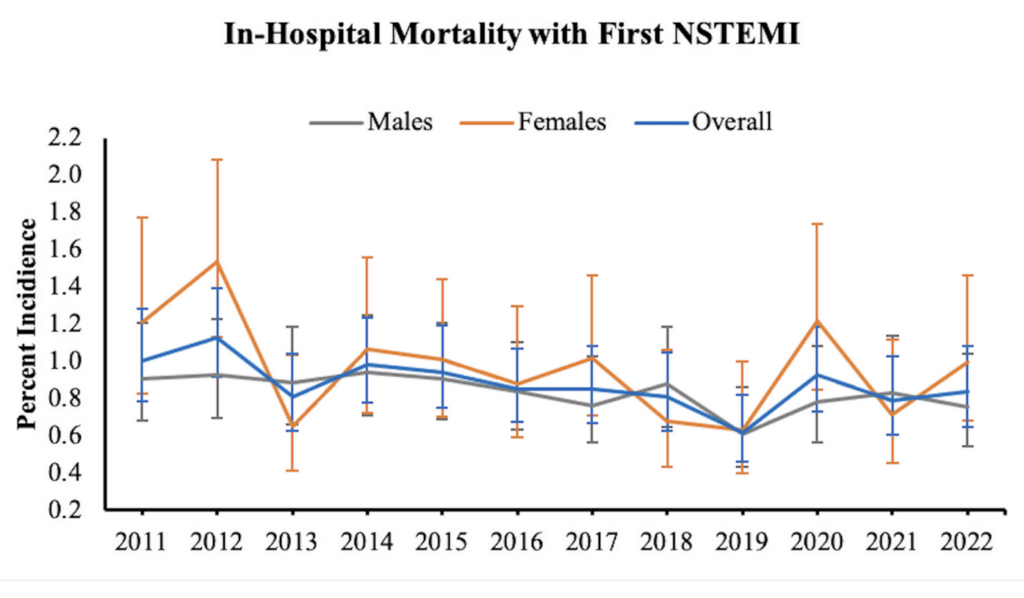
This study also looked at what percentage of young people who had heart attacks died in hospital as opposed to how many heart attacks young people had. It could be that the number of heart attacks is actually going down but that hospitals are providing crappier care. It could be that more young people are making it to the hospital before they die (instead of dying at home). You can’t tell from this article.
Long COVID
This paper from Singapore (2026-01-25) reports that giving early monoclonal antibody (mAb) treatment to unvaccinated, partially vaccinated, and immunocompromised patients in mid-2021 to end 2022 didn’t help and might have hurt. People in the study got Long COVID at the same rate, regardless of whether they got early mAb treatment or not.
😬 Worse, people who got early mAb treatment had a 120% higher risk of autoimmune diseases, especially lupus and rheumatoid arthritis.
Transmission
🐁 Good news! This paper from USA (2025-12-20) looked for COVID-19 in wild white-footed mice between Nov 2023-Jan 2024 in the Northeastern US and couldn’t find any! (They found lots of coronaviruses, just not COVID-19.)
It’s not that white-footed mice don’t ever get COVID: this earlier study (2023-12-13) of in the same region between 2020 and 2022 found COVID-19 in 1% of white-footed mice. This study (2024-07-29) found COVID-19 seroprevalence in 17% of white-footed mice in a mid-Atlantic region between 2022 and 2023.
The researchers also experimented with infecting the mice with various pathogens, and found that they could infect the mice with COVID Classic and Omicron, but that the viral load was way lower in Omicron. Importantly, the infected mice could transmit COVID Classic to uninfected mice but they could not transmit Omicron to uninfected mice.
It looks as if COVID-19 got more optimized for humans as time went on, and that made it de-optimized for non-humans. This is good not just because “save Bambi” but also because this reduces the risk that COVID-19 will mutate inside Bambi and then jump back to us humans.
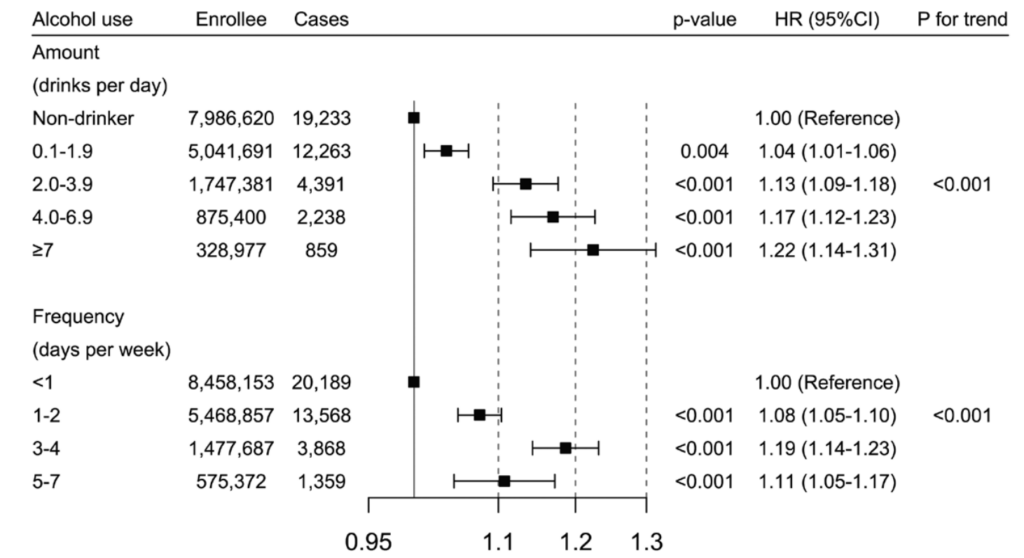
🍻 This paper from South Korea (2026-02-20) reports that the more people drank and the more frequently they drank, the higher their risk of catching COVID-19. The risk of getting a COVID-19 infection increased from a 4% higher (compared to people who didn’t drink) for people who had less than two drinks per day on average up to 22% higher for people who averaged 7 drinks per day.
They looked separately at the frequency of drinking, which makes some sense: maybe the important thing is not “how much alcohol you have” but “how much time you hang out in bars” (famous for being small crowded indoor spaces with poor ventilation). The numbers were a little different here, with the highest risk being for people who drank an average of 3 or 4 times per week (at +19% higher than people who drank less than 1 times per week on average), but people who averaged drinking 5 to 7 days per week only had a +11% higher risk of catching COVID-19. Maybe people who drank every day drank at home instead of going to bars?
🦴 This paper from China (2026-02-18) reports that among people over 55, those who had a COVID-19 reinfection were three times as likely to get a new diagnosis of osteoporosis as those with one infection after adjusting for cofactors.
The reinfected group was about two years older than the once-infected group on average, but the once-infected group didn’t show a strong age-relation. The reinfected group did have a strong age relationship, as you can see in the leftmost four bars in the chart below:
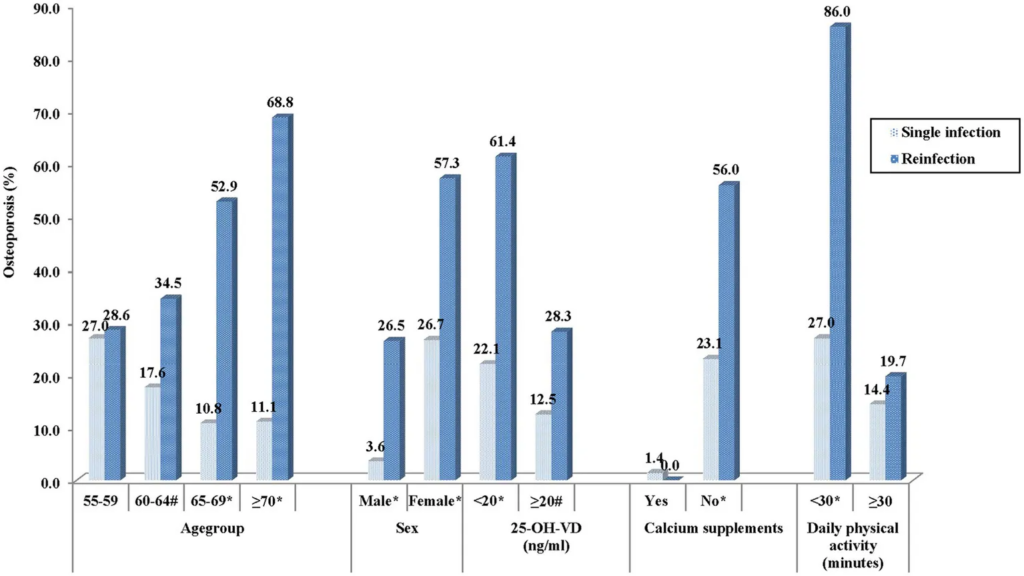
Physical activity, calcium supplements, and high vitamin D levels were also were somewhat protective.
Pathology
👶 This paper from China (2026-02-20) found that babies who had been exposed to COVID-19 in the womb had double the risk of birth defects compared to babies with no COVID-19 exposure, and triple the risk of cardiovascular system malformations.
Vaccines
🤰This paper from Canada (2025-12-15) reports that pregnant people who were not vaccinated had a 3.82 times higher risk of hospitalization during Omicron than those who were vaccinated; during Delta, the unvaccinated had an adjusted risk of 2.43 times the unvaccinated.
Mitigation Measures
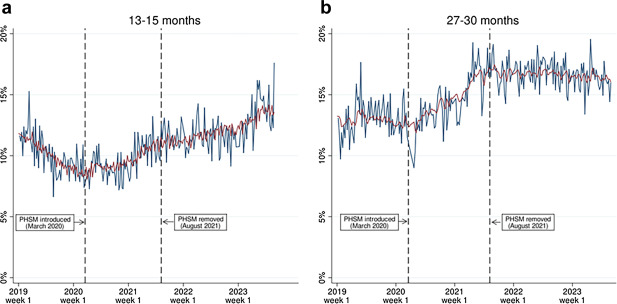
This paper from Scotland (2025-11-25) reports that when public health and safety mitigation measures (PHSM) were implemented, the rate of toddlers getting diagnosed with developmental concerns increased; when mitigation measures were removed, the rate decreased for older toddlers but not younger toddlers.
This paper from California (2025-11-20) reports that the number of mental health diagnoses in school-aged children dropped by 1.2% when the schools reopened.
Treatments
💊 This paper from USA (2025-12-13) reports that employees who got Paxlovid after a COVID-19 infection had 5% fewer sick days, 17% fewer short-term disability days, and 27% fewer long-term disability days than people who did not get Paxlovid.
Recommended Reading
This article (2026-02-17) compares living in a world where COVID-19 exists to living in a world where sexually transmitted diseases exist. It’s an interesting way to frame the issue.
Measles
Costs
💸 Measles isn’t just a health risk for unvaccinated people, it’s also a financial risk for our health care system! This preprint from USA (2026-02-20) estimates that the cost of measles in the USA in 2025 was USD$244.2 million. They estimated that if the vaccination rate number of kids under 7 dropped by 1% per year, it would lead to costs of USD$1.5 billion (with a B!) by 2030.
Transmission
According to the Government of Canada Measles and Rubella Monitoring Report (updated 2026-02-23), in the week ending 14 February 2025, the following jurisdictions had the following number of measles cases:
- Canada: 62;
- Manitoba: 42;
- Alberta: 8;
- Nova Scotia: 7;
- Saskatchewan: 3
- BC: 2.
