COVID
Long COVID
🚑 This paper from USA (2025-12-03) reports that veterans who were eventually diagnosed with Long COVID had a 34% higher risk of emergency department visits in the six months after their infection compared to those who tested positive for COVID-19 infections but who did not get Long COVID.
🩸 This paper from USA (2025-12-05) reports that the risk of a blood clotting event was 75% higher for adults with Long COVID than for adults who had COVID-19 infections but not Long COVID.
👁️ This paper from Germany (2025-11-28) reports that, among people who had laboratory-confirmed COVID-19 infections, the foveal avascular zone (FAZ) of the eyes of people with fatigue was significantly enlarged compared to an unfatigued group. (Their FAZes were also enlarged compared to a healthy control group). People with extreme fatigue had greater macular vascular density than both the no-fatigue group and the control group.
Maybe looking at people’s eyes could be an easy way to diagnose Long COVID.
🧬 This preprint from UK (2025-12-03) did a careful look at the genetics of a lot of people who have ME/CFS, and found a boatload (7,555!) of genetic variants which are implicated. They found genes associated with four different disease mechanisms: neurological dysregulation, inflammation, cellular stress response, and calcium signaling. This strongly suggests that ME/CFS isn’t one thing, and that treatments/trials need to look at subgroups.
They also found a strong but not complete overlap with Long COVID: 76 of 180 genes previously linked to long COVID were also linked to ME/CFS in this study.
👃 This paper from France (2025-12-05) reports that people with Long COVID with smell disruption had significantly worse handwriting metrics than healthy controls. They had significantly inferior average pressure, maximum pressure, average speed, and average jerk (as measured by a tablet computer). A comparison group with Alzheimer’s Disease or mild cognitive impairment had better average pressure and maximum pressure than the patients with a smell disruption.
I couldn’t tell (because paywall) if they selected the smell disruption participants also for other issues (e.g. cognition, fatigue, etc.) or if the only problem the smell disruption participants thought they had was smell.
COVID-Related Excess Sickness and Death
☠️ This paper from Israel (2025-11-13) reports that all-cause mortality for people over 40 after a COVID-19 hospitalization was 69% higher than for a matched cohort which was not hospitalized for COVID-19. It was worse for people between 40 and 64: the hospitalized had a 131% greater chance of dying than the unhospitalized.
Getting at least two doses of vaccine dropped the all-cause mortality risk for those hospitalized by 48% compared to those who did not get vaccinated.
🩸 This paper from China (2025-12-04) reports that COVID-19 has had long-lasting effects on a large population exposed within a short period of time. The authors found that levels of various lymphocyte — T cells, CD4+T cells, CD8+T cells, NK cells, and B cells — dropped significantly and suddenly in the Shandong population when the Chinese government suddenly abandoned their harsh mitigation measures. The lymphocytes rebounded to close to their pre-mass-infection level, but not quite. For example, 20 months later:
- CD4+ T cells were still ~4.4% below baseline;
- CD8+ T cells were still ~9.9% below baseline;
- CD4+ T cells were still ~4.4% below baseline.
It was worse in women and people over 40, but really bad for people with pre-existing cardiovascular disease. After 20 months, in people with pre-existing CVD:
- Total T cells were still 72.9% below baseline;
- CD4+ T cells were still 74.1% below baseline;
- CD8+ T cells were still 68.6% below baseline;
- NK cells were still 46.3% below baseline;
- Total T cells ~5.2% below baseline
🧠 This paper from Saudi Arabia (2025-12-19*) reports that people get diagnosed with mental illnesses a lot more in the four years after a COVID-19 infection. The risks of various illnesses among people with documented COVID-19 infections compared to matched controls was:
- dementia: almost 4 times higher;
- substance use disorder: +95% higher;
- cognitive deficit: +54% higher;
- anxiety disorder: +39% higher;
- mood disorder: +16% higher;
- nerve plexus disorder: +13% higher.
*Yes, I know it’s not Dec 19 yet, but that’s the date that’s listed on the article as the publication date. 🤷♀️
Vaccines
💉 Myocarditis is a rare but genuine risk from mRNA vaccines, especially in young men. (Remember though: the risk of myocarditis from a COVID-19 infection is much higher!) This paper (2025-12-10) reports that the specific cytokines CXCL10 and IFN-γ — players in the innate immune system — caused the inflammation. What’s even better is that they found that genistein (a soybean derivative which binds to estrogen receptors) reduces the risk of myocarditis.
💉 Long-term readers of this blog know I like to point out as often as I can that a vaccination against X offers protection against Y (e.g. flu vaccines reduce the risk of heart attacks). Well, this paper from UK (2025-12-05) says that getting a flu shot does not reduce your risk of Parkinson’s Disease. Vaccines will not fix everything, alas.
💉 This report from US CDC (2025-12-11) says that the 2024–2025 COVID-19 vaccination were quite protective for kids. The six-month VE against emergency department or urgent care was:
- 76% for kids aged 9 months to 4 years;
- 56% for kids aged 5 to 17 years.
💉 This paper from Hong Kong (2025-12-03) reports several things about vaccination in the BA.4/BA.5 timeframe:
- Pfizer’s BNT162b2 booster was 9-21% more effective than CoronaVac;
- the bivalent COVID Classic + BA.4/BA.5 was 30-58% more effective than a COVID Classic booster;
- vaccination-before-infection was more effective than infection-before-vaccination;
- infection-acquired immunity was inferior to vaccine-acquired immunity.
Transmission
🏥🤧 I just discovered this page from PHAC which, among other things, shows what percent of people caught the Big Three respiratory diseases (COVID-19, flu, RSV) in a hospital. It’s sobering.
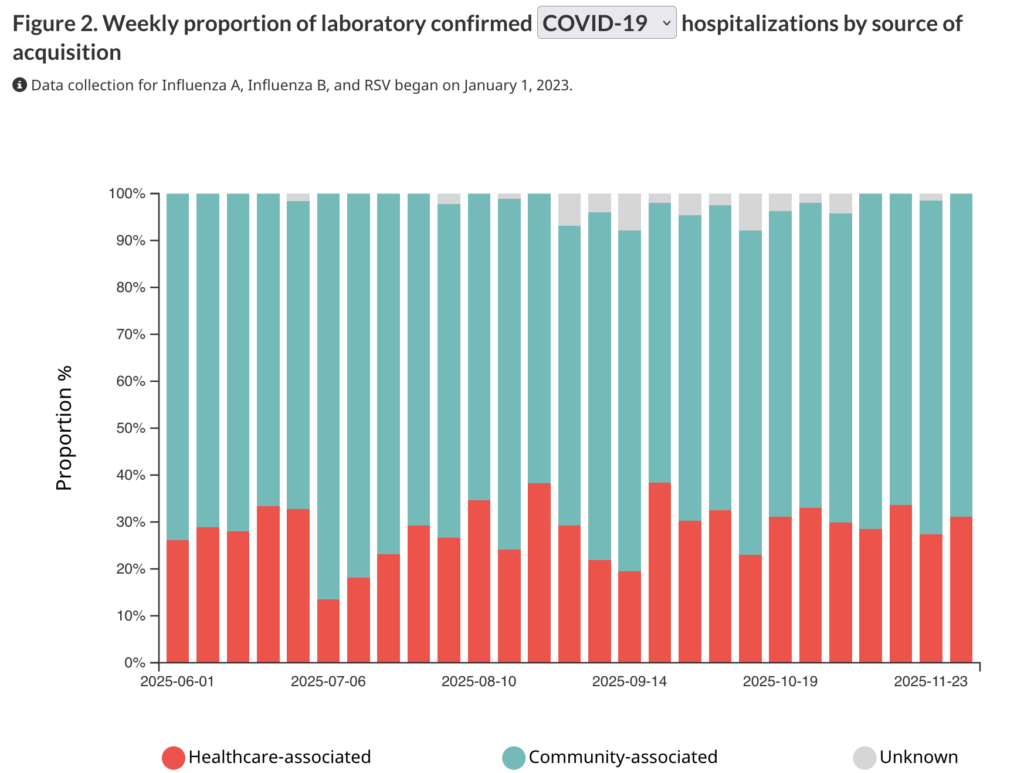
Eyeballing the graph, it looks to me like about a quarter of COVID-19 hospitalizations come from catching COVID-19 in a health-care setting.
😷 Y’all! Wear masks when you go to the doctor!!
Treatments
💊 This not-final paper (2025-12-12?) reports the COVID-19 spike protein S1 pre-treated with aspirin was not as damaging as untreated S1 in either test tubes or inhaled by mice with human immune systems. (Yes, S1 by itself in the bloodstream is damaging. S1 from vaccines is supposed to stay in the lymph system.)
I find this a little odd because there is prior research which has really mixed findings:
- this paper from Poland (2024-02-28) found that patients who had been treated with anti-platelet medications (aspirin or clopidogrel/ticagrelor/prasugrel) before they were hospitalized with COVID-19 did better than matched controls who were not, but
- this paper from Peru (2025-07-11) found that market vendors who self medicated with aspirin increased the risk of COVID-19 infection by 134% compared to those who did not, and
- this preprint from the UK (2021-06-08) found that giving aspirin to hospitalized patients didn’t make a whit of difference to their recovery.
Recommended Reading
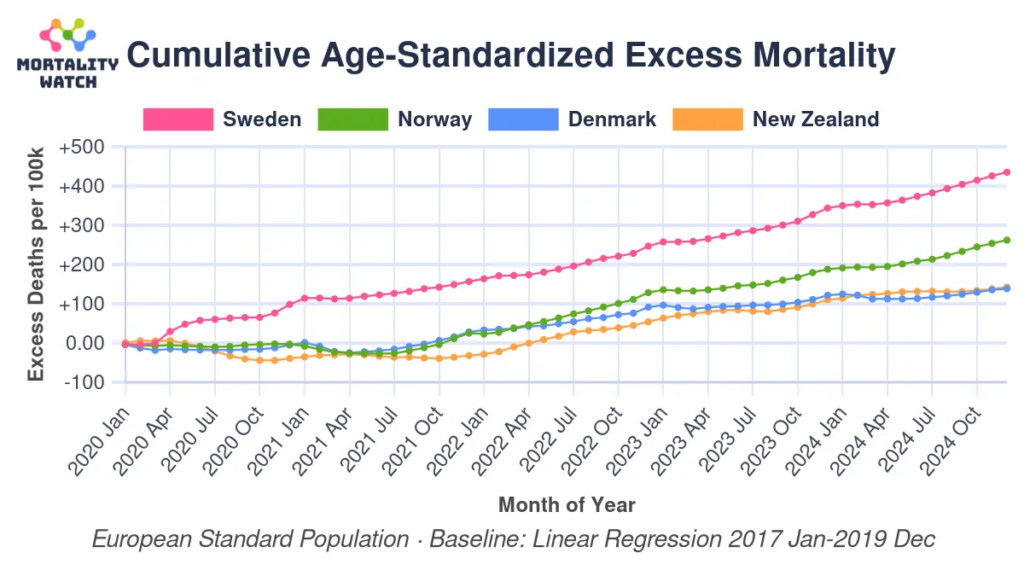
This blog post (2025-11-16) shows how — depending upon how you choose the baseline to compare against — you can pretty easily manipulate excess death statistics. Compare two different graphs with different baselines: a linear regression baseline and a straight-average baseline:
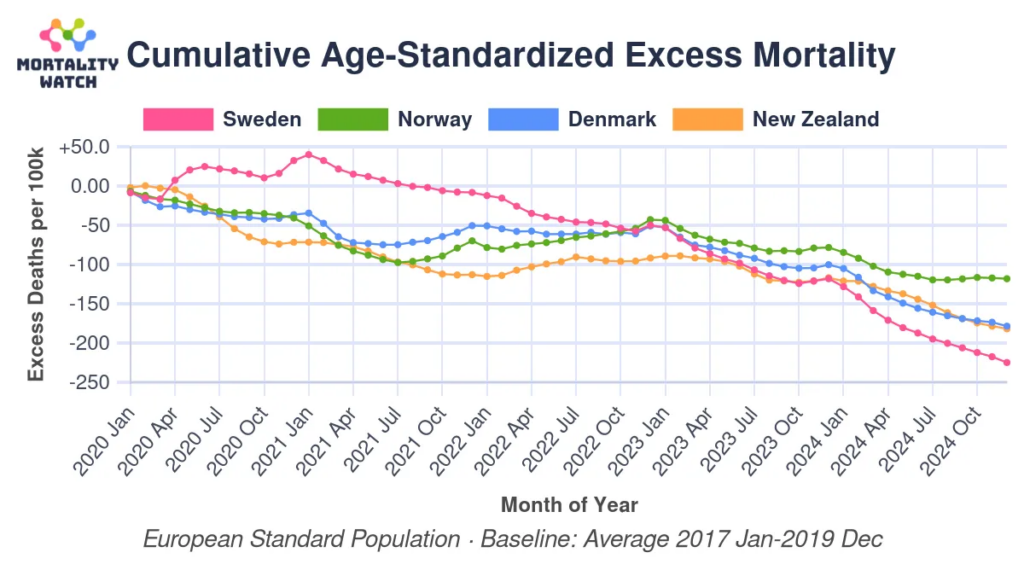
RSV
Pathology
🫀 This paper from UK (2025-12-08) reports that adult participants over 45 years old who had an RSV infection were 2.7 times more likely to have a cardiovascular event in the next year than people who did not have RSV.
Measles
Transmission
According to the Government of Canada Measles and Rubella Monitoring Report (updated 2025-12-01), in the week ending 22 November, the following jurisdictions had the following number of cases:
- Canada: 37;
- Manitoba: 12;
- Saskachewan: 11;
- Alberta: 7;
- BC: 6;
- Quebec: 1.
