COVID-19
Long COVID
‼️‼️‼️🎉🎉🎉This article (2025-07-22) and this paper from Canada (2025-07-07) say that scientists have found a really easy blood test to diagnose ME/CFS! (They look for the protein SMPDL3B.)
This is both great for testing purposes but also suggests a treatment!
They haven’t looked for SMPDL3B in Long COVID patients yet, but I think that’s just because they were busy finishing their ME/CFS work.
🎉 This paper from USA (2025-07-22) reports that some people at pulmonary Long COVID clinic had ACE2-like abzymes (also called catalytic monoclonal antibodies, a monocolonal antibody that acts as a catalyst). They think that the antibodies these people make for the receptor binding domain (RBD) look a lot like ACE2 — the enzyme that the ACE2 receptor recognizes.
Why does the body make antibodies that look like ACE2 instead of looking like the ACE2 receptor? They suggest that the body makes antibodies to the antibodies which do look like the ACE2 receptor!
ACE2, like many parts of the human microbiology, has multiple uses, and one of the things it does is help regulate blood pressure. The authors of the paper found that ACE2-like activity correlated with abnormal blood pressure changes in an exercise test.
This suggests both how to test for Long COVID and how to treat it.
This paper from USA (2025-07-23) reports that the risk of developing new-onset CFS/ME was higher among people who had COVID-19 than those who did not: 46% higher among those who were hospitalized for it and 56% higher for those who were not hospitalized. (No, I don’t understand how a lower severity case of COVID-19 would have a lower risk. This conflicts with many other studies.)
They also reported the risk difference for many other conditions, but they did a crappy job of saying what the comparison was against. Against people who never had COVID-19? Against people with COVID who did not have the condition? Here are the increased risks for a number of conditions, though I don’t know how much they mean without knowing what it’s higher relative to:
- having had a COVID-19 vaccination: 24% higher risk (which conflicts with other studies);
- being female: +54%;
- having an autoimmune disease: +57%;
- having a depressive disorder: +28%;
- having anxiety disorder: +35%;
They said that the risk of incident CFS/ME was not associated with age, most comorbidities, insurance, or neighborhood median income.
This paper from USA (2025-07-11) categorized patients who had had confirmed COVID-19 and later had complaints about their cognition. The authors classified them into three groups:
- Profile 1: Widespread generalized cognitive issues and daily fatigue;
- Profile 2: Widespread generalized cognitive issue (but not as bad as Profile 1 and less fatigue);
- Profile 3: a specific impairment of verbal long-term memory and fewer complaints. This group was mostly men.
🎉 This dissertation from Germany (2025-07-22) reports that levels of YKL-40 correlate with Long COVID symptoms.
🧠 This article (2025-06-22) about this paper (2025-06-20) says that people with Long COVID have very specific memory difficulties compared to healthy controls:
- much worse ability to form memories when distracted;
- worse ability to distinguish between similar memories.
COVID-Related Excess Sickness and Death
🦟 This paper from India (2025-07-19) found evidence that COVID-19 messes with your immune system:
- People with dengue and a history of COVID-19 were FIFTY-SIX TIMES as likely to have a severe case of dengue than people who had dengue and no history of COVID-19.
- People with malaria and a history of COVID-19 were TWO HUNDRED AND SIXTY-FOUR TIMES as likely to have a severe case of malaria than people who had malaria and no history of COVID-19.
Pathology
🧠 This paper from UK (2025-07-22) reports that the pandemic aged people’s brains, even if they did not catch COVID-19. (If they caught COVID-19, then they scored worse on cognitive tests than those who did not.)
The used MRI and cognitive test data from the UK BioBank project, and fed that into AIs. They first used AIs to figure out the biological age of the brains from pre-pandemic MRIs of people of different ages. They then compared
- MRI scans from people who had two scans before the pandemic with
- scans from people who had one scan before and one after the start of the pandemic.
They further broke down the post-pandemic group into those who’d had COVID-19 and those who had not. They found that there wasn’t any significant difference in accelerated brain aging between the post-pandemic-had-COVID and post-pandemic-didn’t-have-COVID groups, but there was a difference in the pre-pandemic and post-pandemic groups. The post-pandemic cohort had brains which had aged about 5.5 months more (on average) than the matched pre-pandemic cohort.
Accelerated brain aging was worse in men, people from lower sociio-economic backgrounds, and older age.
They then compared results of cognitive tests in the various cohorts and found that the post-pandemic-had-COVID cohort scored worse on average than the post-pandemic-didn’t-have-COVID cohort. The pre-pandemic cohort and the post-pandemic-didn’t-have-COVID cohort did not have a significant difference in cognitive results.
What I’d conclude from these results is:
- Everybody was traumatized by the conditions of the pandemic, and that trauma aged our brains;
- COVID-19 makes you stupider, but the pandemic trauma did not, despite the brain aging.
NB: I don’t know how the UK BioBank decides if people have had COVID-19 or not. If they didn’t do antibody tests, then they don’t actually know who had COVID-19 and who did not.
☀️ This paper from UK (2025-07-18) reports that low Vitamin D slightly reduces the chances of getting a COVID-19 infection, but increases the risk of hospitalization by a bit more:
- Overall, a Vitamin D insufficiency reduced the risk of a COVID-19 infection by 3%.
- Overall, a Vitamin D deficiency reduced the risk of a COVID-19 infection by 5%.
- Overall, a Vitamin D insufficiency increased the risk of a hospitalization for COVID-19 by 19%.
- Overall, a Vitamin D deficiency increased the risk of a hospitalization for COVID-19 by 36%.
- The numbers were worse for subgroups with darker skin:
- For Asian people, a Vitamin D deficiency gave a 50% higher risk of COVID-19 infection;
- for Black people, a Vitamin D deficiency gave a 57% higher risk of COVID-19 infection.
😬🐹🧠 This study (2025-07-22) found that hamsters infected with COVID-19 had replication-competent virus in their brains 80 days later.
Testing
💩💧 This older paper from USA (2022-10-03) found that the amount of virus shed in wastewater per person was highest for Delta and lowest for Omicron. They wondered if maybe the amount of virus shed was related to how severe the disease was (since Delta was the nastiest and Omicron was the mildest.)
BC Wastewater
💩💧 It looks like the BC wastewater is going down again, or at least holding steady.
From Jeff’s wastewater spreadsheet:
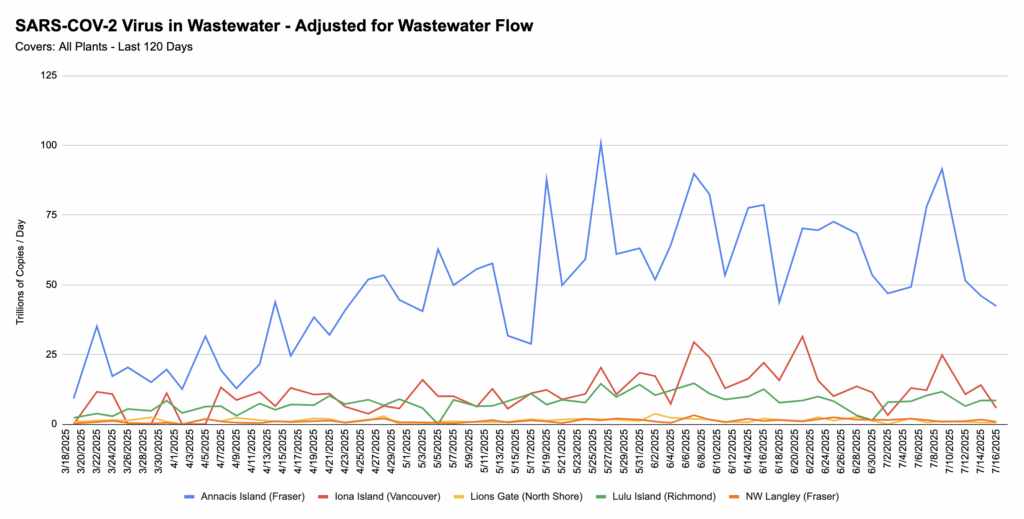
Recommended Reading
Some of you might remember that there was a drug called BC 007 which looked very promising as an anti-Long COVID drug, but which flunked its Phase 2 trial. (I was quite sad to see that it didn’t pass the Phase 2 trial because it looked so promising!) This article (2025-07-22) looks at the Phase 2 trial in depth, and asserts that the Phase 2 trial was just designed poorly: it didn’t select its participants carefully enough, the tests required from the study were onerous enough that they could have caused people to get worse, and they didn’t choose the right success metrics.
🎉 The good news is that this preprint from Germany (2024-12-14) reports that a smaller, better-designed study, found that BC007 did significantly improve Long COVID patients’ quality of life.
Sudan Virus
Pathology/Long Sudan Virus
This paper from Uganda (2025-07-18) says that half of the people in their study of Sudan ebolavirus survivors had persistent multi-systemic symptoms badly enough that it interfered with the basic activities of living. Also, they found viral RNA in breast milk and semen for about 200 days. 😬
H5N1
Transmission
🐦⬛😷 Why isn’t H5N1 a bigger problem in humans? This paper (2025-07-22) suggests that it’s prior exposure to related influenza viruses. Ferrets who were deliberately infected with H1N1 or H2N3 (by scientists), then later were deliberately infected with H5N1 (by scientists) had milder disease than those who didn’t get exposed to either before getting infected with H5N1. The H2N3-exposed ferrets got sicker on average than the H1N1-exposed ferrets, but none of the ferrets with prior immunity died; all of the ferrets who did not have prior immunity died.
Having previous exposure to H1N1 also kept the ferrets from catching H5N1 from cohoused ferrets infected with lethal amounts of H5N1. And while ferrets pre-exposed to H3N2 did get sick from their cagemates, the previous exposure was about 50% protective — only half of the previously-exposed-to-H3N2 ferrets died.
So if you are worried about bird flu? Go get an influenza vaccine!
Dang, and I had hoped H5N1 was petering out. This article (2025-07-23) says that two more dairy herds in California have tested positive for H5N1. There have been 1777 detected-infected herds in 17 states, with 770 herds just in California. (That makes sense; it’s the biggest state, and — being a Democratic state — they are probably actually testing instead of burying their heads in the sand.)
Mpox
Transmission
This article (2025-07-24) doesn’t put it in exactly those words, but mpox is getting out of control in Africa. Part of the problem is that they have run out of donated vaccine doses. Bavarian Nordic has 800,000 doses on the shelf, but organizations like UNICEF don’t have the money to buy them. (Africa CDC also estimates that they need 3.4M doses.)
This is so f short-sighted. Aside from the humanitarian tragedy, if it isn’t curtailed in Africa, the rest of the world won’t be able to contain it! How much will it cost to vaccinate 8 billion people vs. 3.4 million???? (I’ll do the math for you: 2353 times more.)
Measles
Transmission
The Government of Canada web page on measles (2025-07-31) says that in the week ending 12 July 2025, there were 158 new cases nationally, including:
- 81 in Alberta;
- 35 in Ontario;
- 16 in Manitoba;
- 13 in BC.
